Prostate Conditions
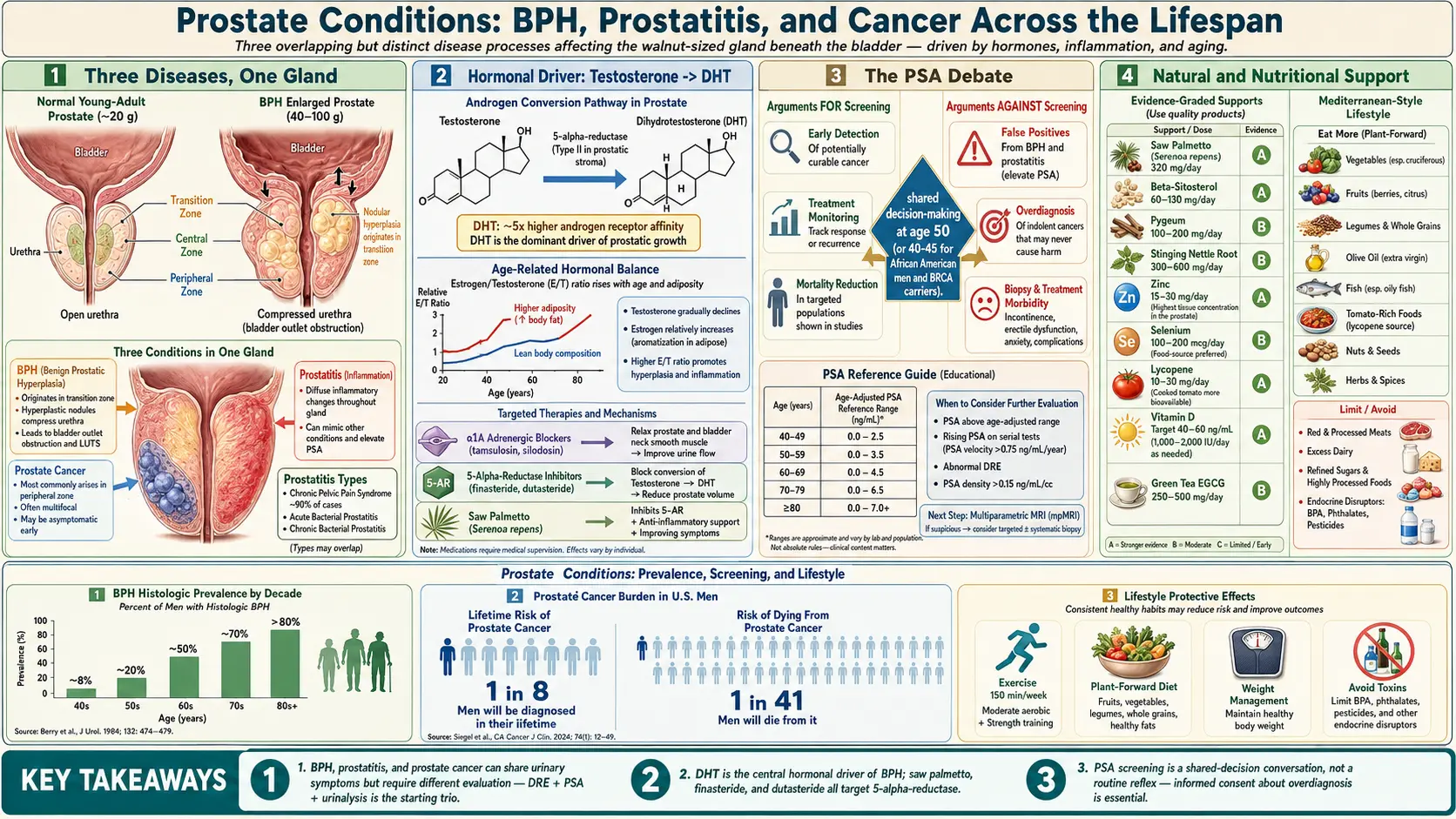
Table of Contents
- Overview of the Prostate
- Benign Prostatic Hyperplasia (BPH)
- Prostatitis
- Prostate Cancer Screening and the PSA Debate
- Risk Factors
- Common Symptoms
- Conventional Treatments
- Natural Support for Prostate Health
- Diet and Lifestyle Modifications
- Pelvic Floor Health
- Cautions and When to Seek Medical Care
- References & Research
- Research Papers
- Connections
- Featured Videos
Overview of the Prostate
The prostate gland is a walnut-sized organ located below the bladder and surrounding the urethra in men. It produces seminal fluid that nourishes and transports sperm. As men age, the prostate is susceptible to several conditions that can significantly impact urinary function and quality of life. From a naturopathic perspective, prostate health is deeply connected to hormonal balance, nutritional status, and overall metabolic wellness.
Benign Prostatic Hyperplasia (BPH)
Benign prostatic hyperplasia is a non-cancerous enlargement of the prostate gland that affects the majority of men as they age. By age 60, roughly half of all men have some degree of BPH, and by age 85, approximately 90% are affected.
How BPH Develops
BPH is driven primarily by the conversion of testosterone to dihydrotestosterone (DHT) by the enzyme 5-alpha reductase. DHT stimulates prostate cell growth. Estrogen levels also rise relative to testosterone with aging, which may further promote prostate tissue proliferation. Chronic low-grade inflammation is increasingly recognized as a contributing factor.
Symptoms of BPH
- Frequent urination, especially at night (nocturia)
- Weak or interrupted urine stream
- Difficulty initiating urination (hesitancy)
- Sensation of incomplete bladder emptying
- Urgency and occasional urge incontinence
- Dribbling at the end of urination
Prostatitis
Prostatitis refers to inflammation of the prostate gland and is the most common urological diagnosis in men under 50. It can be acute or chronic, bacterial or non-bacterial.
Types of Prostatitis
- Acute bacterial prostatitis: Sudden onset with fever, chills, painful urination, and pelvic pain. Requires prompt antibiotic treatment.
- Chronic bacterial prostatitis: Recurring bacterial infections with milder but persistent symptoms.
- Chronic pelvic pain syndrome (CPPS): The most common form, accounting for roughly 90% of cases. No identifiable bacterial cause but involves chronic pelvic pain, urinary symptoms, and sometimes sexual dysfunction.
- Asymptomatic inflammatory prostatitis: Inflammation found incidentally during evaluation for other conditions.
Naturopathic practitioners often address CPPS through a combination of anti-inflammatory nutrition, stress management, pelvic floor rehabilitation, and targeted supplementation.
Prostate Cancer Screening and the PSA Debate
The prostate-specific antigen (PSA) test has been a cornerstone of prostate cancer screening since the late 1980s, but it remains one of the most debated topics in men's health.
Arguments for PSA Screening
- Can detect prostate cancer at an early, potentially curable stage
- Useful for monitoring men already diagnosed with prostate cancer
- May reduce prostate cancer mortality when used in targeted populations
Arguments Against Routine PSA Screening
- High false-positive rate: PSA can be elevated due to BPH, prostatitis, recent ejaculation, or cycling
- Overdiagnosis: Many prostate cancers are slow-growing and may never cause symptoms or death
- Overtreatment risks: Unnecessary biopsies, surgeries, and radiation carry significant side effects including incontinence and erectile dysfunction
An informed, shared decision-making approach is recommended. Men should discuss the potential benefits and harms with their healthcare provider, especially beginning at age 50 (or 40-45 for higher-risk individuals).
Risk Factors
- Age: The single greatest risk factor for all prostate conditions
- Family history: Having a first-degree relative with prostate cancer doubles the risk
- Ethnicity: African American men have higher rates of prostate cancer and BPH
- Hormonal imbalances: Elevated DHT and estrogen-to-testosterone ratio
- Obesity: Associated with more aggressive prostate disease and higher estrogen levels
- Sedentary lifestyle: Contributes to pelvic congestion and metabolic dysfunction
- Chronic inflammation: Poor diet, environmental toxins, and chronic stress all promote systemic inflammation
- Exposure to endocrine disruptors: BPA, phthalates, and pesticides may affect prostate health
Common Symptoms
While specific symptoms vary by condition, the following are general warning signs that warrant evaluation:
- Changes in urinary frequency or urgency
- Pain or burning during urination
- Blood in urine or semen
- Pelvic, lower back, or perineal pain
- Painful ejaculation
- Erectile dysfunction
- Unexplained weight loss (potential cancer sign)
Conventional Treatments
For BPH
- Alpha-blockers (tamsulosin, alfuzosin): Relax smooth muscle in the prostate and bladder neck
- 5-alpha reductase inhibitors (finasteride, dutasteride): Block DHT production to shrink the prostate
- Combination therapy: Alpha-blocker plus 5-alpha reductase inhibitor for moderate to severe BPH
- Minimally invasive procedures: UroLift, Rezum water vapor therapy, transurethral microwave thermotherapy
- Surgery: Transurethral resection of the prostate (TURP) for severe cases
For Prostatitis
- Antibiotics: For bacterial forms (fluoroquinolones, trimethoprim-sulfamethoxazole)
- Alpha-blockers: To relieve urinary symptoms
- Anti-inflammatories: NSAIDs for pain management
- Physical therapy: Pelvic floor myofascial release for CPPS
Natural Support for Prostate Health
From a naturopathic perspective, several evidence-based natural therapies can support prostate health, either as primary approaches for mild conditions or as complementary support alongside conventional care.
Saw Palmetto (Serenoa repens)
Saw palmetto is the most well-researched herbal remedy for BPH. It works as a mild 5-alpha reductase inhibitor, reducing DHT levels in prostate tissue. It also has anti-inflammatory and anti-estrogenic properties. Clinical studies suggest it can improve urinary symptoms and flow rates in men with mild to moderate BPH. A typical dosage is 320 mg daily of a standardized liposterolic extract.
Beta-Sitosterol
Beta-sitosterol is a plant sterol found in many fruits, vegetables, nuts, and seeds. Multiple randomized controlled trials have shown it significantly improves urinary symptom scores and flow measures in men with BPH. It works through anti-inflammatory mechanisms and may also inhibit 5-alpha reductase.
Pygeum (Prunus africana)
Pygeum bark extract has been used in European medicine for decades to treat BPH symptoms. It reduces inflammation, inhibits growth factors that promote prostate cell proliferation, and may improve bladder contractility. Standard dosage is 100-200 mg daily.
Stinging Nettle Root (Urtica dioica)
Stinging nettle root is often combined with saw palmetto for synergistic effects. It appears to inhibit the binding of DHT to sex hormone-binding globulin (SHBG) and may have anti-aromatase activity. It also contains anti-inflammatory lignans.
Zinc
The prostate gland contains the highest concentration of zinc of any organ in the body. Zinc levels are significantly reduced in both BPH and prostate cancer tissue. Adequate zinc intake (15-30 mg daily) supports normal prostate cell function and may help regulate DHT metabolism. Excessive zinc supplementation (over 40 mg daily) should be avoided as it can impair copper absorption.
Selenium
Selenium is an essential trace mineral with antioxidant properties. Some observational studies have linked adequate selenium status with reduced prostate cancer risk, though supplementation trials have shown mixed results. Food sources such as Brazil nuts, sardines, and organ meats are preferred over high-dose supplements.
Lycopene
Lycopene, the red pigment found in tomatoes, watermelon, and pink grapefruit, is a potent antioxidant that concentrates in prostate tissue. Epidemiological studies consistently associate higher lycopene intake with reduced prostate cancer risk. Cooked tomato products provide more bioavailable lycopene than raw tomatoes.
Vitamin D
Vitamin D receptors are present throughout prostate tissue, and vitamin D plays a role in regulating cell growth and differentiation. Low vitamin D levels have been associated with increased risk of aggressive prostate cancer. Maintaining optimal vitamin D status (40-60 ng/mL) through sun exposure, diet, and supplementation is recommended.
Green Tea and EGCG
Epigallocatechin gallate (EGCG), the primary catechin in green tea, has demonstrated anti-proliferative and pro-apoptotic effects on prostate cancer cells in laboratory studies. Population studies from Asia show lower prostate cancer incidence among regular green tea drinkers. Drinking 3-5 cups daily or taking a standardized EGCG supplement may provide protective benefits.
Diet and Lifestyle Modifications
Mediterranean Diet
A Mediterranean-style diet rich in vegetables, fruits, whole grains, olive oil, fish, and legumes provides a foundation for prostate health. This dietary pattern is anti-inflammatory, rich in antioxidants, and associated with lower rates of prostate cancer and BPH progression.
- Cruciferous vegetables (broccoli, cauliflower, kale): Contain sulforaphane and indole-3-carbinol, which support healthy estrogen metabolism
- Fatty fish (salmon, sardines, mackerel): Provide omega-3 fatty acids that reduce inflammation
- Pumpkin seeds: Rich in zinc and phytosterols that support prostate health
- Fermented foods: Support gut health, which influences hormonal balance and inflammation
Foods and Substances to Limit or Avoid
- Red and processed meats: Associated with increased prostate cancer risk
- Dairy products: High calcium intake from dairy may be linked to elevated prostate cancer risk
- Refined sugars and processed foods: Promote inflammation and insulin resistance
- Excessive alcohol: Disrupts hormonal balance and liver detoxification
- Caffeine: Can worsen urinary symptoms in men with BPH
Exercise
Regular physical activity is strongly associated with better prostate outcomes. Aim for at least 150 minutes of moderate aerobic exercise per week. Resistance training can help maintain healthy testosterone levels. Exercise also reduces obesity, insulin resistance, and chronic inflammation, all of which are risk factors for prostate disease.
Avoiding BPA and Endocrine Disruptors
Bisphenol A (BPA) and other endocrine-disrupting chemicals can mimic estrogen and interfere with hormonal signaling in the prostate. To minimize exposure:
- Avoid plastic food containers, especially when heating food
- Choose BPA-free canned goods or opt for glass and stainless steel containers
- Filter drinking water to remove contaminants
- Choose organic produce when possible to reduce pesticide exposure
- Avoid personal care products containing parabens and phthalates
Pelvic Floor Health
The pelvic floor muscles play a critical but often overlooked role in prostate-related symptoms, particularly in chronic pelvic pain syndrome and post-surgical recovery.
- Kegel exercises: Strengthening the pelvic floor muscles can improve urinary control, especially after prostate surgery
- Pelvic floor relaxation: For men with CPPS, the pelvic floor is often hypertonic (too tight). Relaxation techniques, diaphragmatic breathing, and stretching are more appropriate than strengthening
- Myofascial release therapy: Internal and external trigger point therapy performed by a trained pelvic floor physical therapist can significantly reduce pain in CPPS
- Stress management: Chronic stress contributes to pelvic floor tension. Practices such as yoga, meditation, and mindfulness can help break the pain-tension cycle
Cautions and When to Seek Medical Care
While natural approaches can be valuable for supporting prostate health, certain situations require prompt medical attention:
- Acute urinary retention (complete inability to urinate) is a medical emergency
- Blood in urine or semen should always be evaluated to rule out serious conditions
- Fever with urinary symptoms may indicate acute bacterial prostatitis or urinary tract infection requiring antibiotics
- Rapidly worsening symptoms or unexplained weight loss warrant thorough medical evaluation
- Herbal supplements such as saw palmetto may interact with blood thinners and hormonal medications
- Do not self-treat suspected prostate cancer with natural remedies alone. Integrative approaches should complement, not replace, appropriate oncological care
- PSA testing: Some supplements (including saw palmetto) may lower PSA levels, potentially masking disease. Inform your physician of all supplements you take
A collaborative approach between naturopathic and conventional providers offers the most comprehensive care for prostate health.
12. References & Research
Historical Background
The prostate gland was first described anatomically by Venetian anatomist Niccolo Massa in 1536. The first prostatectomy was performed by Theodor Billroth in 1867. Hugh Hampton Young developed the perineal prostatectomy technique in 1904, and the prostate-specific antigen (PSA) test was introduced for clinical use in the late 1980s by Thomas Stamey and colleagues, fundamentally changing prostate cancer screening.
Key Research Papers
- Schroder FH, Hugosson J, Roobol MJ, et al. Prostate-cancer mortality at 11 years of follow-up (ERSPC trial). New England Journal of Medicine. 2012;366(11):981-990.
- Andriole GL, Crawford ED, Grubb RL III, et al. Mortality results from a randomized prostate-cancer screening trial (PLCO). New England Journal of Medicine. 2009;360(13):1310-1319.
- Thompson IM, Goodman PJ, Tangen CM, et al. The influence of finasteride on the development of prostate cancer (PCPT). New England Journal of Medicine. 2003;349(3):215-224.
- McConnell JD, Roehrborn CG, Bautista OM, et al. The long-term effect of doxazosin, finasteride, and combination therapy on the clinical progression of BPH (MTOPS). New England Journal of Medicine. 2003;349(25):2387-2398.
- Gravas S, Cornu JN, Gacci M, et al. EAU Guidelines on Management of Non-Neurogenic Male Lower Urinary Tract Symptoms (LUTS) including BPH. European Urology. 2019;75(6):1054-1063.
- Tacklind J, Macdonald R, Rutks I, Stanke JU, Wilt TJ. Serenoa repens for benign prostatic hyperplasia. Cochrane Database of Systematic Reviews. 2012;12:CD001423.
- Lippman SM, Klein EA, Goodman PJ, et al. Effect of selenium and vitamin E on risk of prostate cancer (SELECT trial). JAMA. 2009;301(1):39-51.
- Hamdy FC, Donovan JL, Lane JA, et al. 10-Year outcomes after monitoring, surgery, or radiotherapy for localized prostate cancer (ProtecT trial). New England Journal of Medicine. 2016;375(15):1415-1424.
- US Preventive Services Task Force. Screening for Prostate Cancer: US Preventive Services Task Force Recommendation Statement. JAMA. 2018;319(18):1901-1913.
- Nickel JC. Prostatitis. Canadian Urological Association Journal. 2011;5(5):306-315.
- Roehrborn CG. Benign prostatic hyperplasia: an overview. Reviews in Urology. 2005;7(Suppl 9):S3-S14.
- Wilt TJ, Brawer MK, Jones KM, et al. Radical prostatectomy versus observation for localized prostate cancer (PIVOT trial). New England Journal of Medicine. 2012;367(3):203-213.
Research Papers
- Clinical trials on prostate health (BPH and prostatitis) — PubMed search
- PSA screening and prostate cancer outcomes — PubMed search
- Saw palmetto (Serenoa repens) for prostate health — PubMed search
- Chronic prostatitis / chronic pelvic pain syndrome — PubMed search
- Lycopene and prostate cancer risk — PubMed search
- Zinc and prostate disease — PubMed search
- Pygeum africanum for BPH — PubMed search
- Active surveillance for localized prostate cancer — PubMed search
Connections
- Benign Prostatic Hyperplasia
- Zinc
- Erectile Dysfunction
- Saw Palmetto
- Selenium
- Low Testosterone / TRT
- Urinary Tract Infections
- Cancer Overview
- Testosterone Test
- PSA Test
- Green Tea
- Obesity
- Insulin Resistance
- Tomatoes
- Omega-3 Fatty Acids
- Bladder Cancer
- rBGH
- Selenium and Cancer Prevention
Featured Videos

8 Signs YOU Have an Enlarged Prostate (BPH Symptoms)| Doctor Explains

Why Men Get an Enlarged Prostate and How to Treat BPH Symptoms

Enlarged Prostate Signs, Symptoms, Causes, Treatments (Men's Health) - Tagalog Health | Nurse Dianne

What is PROSTATE CANCER? Doctor explains SIGNS, SYMPTOMS, TREATMENT and more!

Best Ways to Prevent Prostate Enlargement, Explained by a Urologist

Prostate Disorders | Clinical Medicine

Prostate Cancer: Symptoms, Diagnosis, & Treatment | Stanford

Bacteria won't leave your prostate? Do this! | UroChannel

Salamat Dok: Dr. Michael Hernandez discusses the medications and treatments for prostate cancer