CAC, Statins, and the Density Paradox: How Calcium Reshapes Cholesterol Decisions
The single most consequential clinical use of the coronary calcium score is in reshaping the statin decision. CAC turns the abstract "10-year ASCVD risk percentage" into a concrete picture of accumulated plaque, and that visibility changes the conversation: it can confirm the need for therapy, defer it for years, or escalate it past guideline-default intensity. This page covers the guideline thresholds, the trial evidence behind them, and the most counterintuitive finding in the field: statins make your calcium score go up, even as they reduce your risk of dying from a heart attack.
Table of Contents
- Guideline Thresholds for Statin Recommendation
- Deferring Statins with CAC = 0
- The CAC ≥100 Threshold
- High CAC: Aggressive Therapy
- SCOT-HEART Trial
- ROBINSCA Trial
- The Density Paradox
- Progression on Statins
- Beyond Statins
- Research Papers and References
- Connections
- Featured Videos
Guideline Thresholds for Statin Recommendation
The 2018 ACC/AHA cholesterol guideline (and subsequent updates) explicitly incorporate CAC into the statin decision pathway for primary prevention. The relevant cutoffs:
- CAC = 0 — Reasonable to defer statin therapy in adults at intermediate ASCVD risk (5–19.9%) without diabetes, smoking, or family history of premature CAD
- CAC 1–99 — Statin reasonable, especially in those at higher percentiles for age
- CAC ≥100 OR ≥75th percentile — Statin recommended regardless of LDL-C level
- CAC ≥300 — High-intensity statin; consider aspirin if not contraindicated; aggressive risk-factor management
Different societies have slightly different thresholds. The European ESC guideline emphasizes percentile rather than absolute number. The American College of Cardiology favors the absolute ≥100 cutoff for simplicity.
Deferring Statins with CAC = 0
The deferral pathway is one of the strongest reasons to obtain a CAC. Patients with intermediate ASCVD risk but a calcium score of zero have 10-year event rates so low that the absolute benefit of statin therapy becomes very small — the number-needed-to-treat over a decade is in the 200–400 range, comparable to many other interventions whose risk/benefit balance favors deferral.
Practical interpretation: a 60-year-old with LDL-C 145, no diabetes, no smoking, no family history, and a CAC of 0 has <1% 10-year event risk. Standard pooled-cohort risk calculation might suggest 8–10% risk and trigger a statin recommendation. The CAC = 0 result reasonably defers that recommendation with a re-evaluation timeline of 5–10 years. See the CAC = 0 page.
The CAC ≥100 Threshold
A CAC score of 100 or above triggers statin recommendation in most current guidelines, regardless of LDL-C level or pooled-cohort risk score. The reasoning:
- 10-year event rates approach or exceed 7.5% at CAC ≥100, meeting threshold for statin benefit
- The presence of mature plaque means the lipoprotein-driven atherogenic process has advanced; further LDL exposure compounds the existing burden
- Statin therapy reduces 10-year MI and CV death by 25–35% in this population
- The number-needed-to-treat over a decade falls to ~30–50, a clearly favorable risk/benefit balance
This threshold has shifted clinical practice meaningfully — many patients who would not have qualified for statins under older LDL-C-only criteria now qualify based on calcium burden, and many patients who would have been pressured into therapy on borderline calculator results are now reasonably watched.
High CAC: Aggressive Therapy
For CAC ≥300, especially ≥1000 or top-percentile-for-age:
- High-intensity statin (atorvastatin 40–80 mg or rosuvastatin 20–40 mg) — aim for LDL-C <70 mg/dL or 50% reduction
- Consider ezetimibe if LDL-C target not met on statin alone
- Consider PCSK9 inhibitors in genetic dyslipidemia or persistent very-high LDL despite statin + ezetimibe
- Aspirin 81 mg daily often appropriate (after weighing bleeding risk), especially in high-risk patterns
- Tight blood pressure control — goal <130/80
- Diabetes screening and management — SGLT2 inhibitors and GLP-1 agonists if diabetic
- Stress test or CCTA if symptoms emerge or as a one-time anatomy/ischemia evaluation
- Cardiology consultation at very high scores
SCOT-HEART Trial
The SCOT-HEART trial (Lancet, 2018) randomized 4,146 Scottish patients with stable chest pain to standard care vs CCTA-guided care. Five-year results:
- CCTA-guided arm: 41% relative reduction in death from CHD or non-fatal MI (HR 0.59, 95% CI 0.41–0.84)
- The benefit was driven by more accurate diagnosis and earlier statin initiation in the CCTA arm
- The trial demonstrated that imaging-guided care, beyond just CAC, can reduce hard endpoints
SCOT-HEART used CCTA, not pure CAC, but the principle — that visualization of plaque changes management in a way that improves outcomes — underlies the use of CAC in primary prevention as well.
ROBINSCA Trial
ROBINSCA (Risk Or Benefit IN Screening for CArdiovascular disease) was a large Dutch trial randomizing asymptomatic adults at moderate baseline risk to no screening, ASCVD-risk-score-based management, or CAC-based management. Findings:
- CAC-based screening identified more high-risk patients earlier than ASCVD-risk-only management
- Patients with elevated CAC who started statins earlier had better long-term cardiovascular outcomes
- The trial supported population-level CAC screening for asymptomatic adults at intermediate baseline risk
ROBINSCA, alongside SCOT-HEART, has been influential in moving CAC from "interesting research test" into mainstream primary prevention practice.
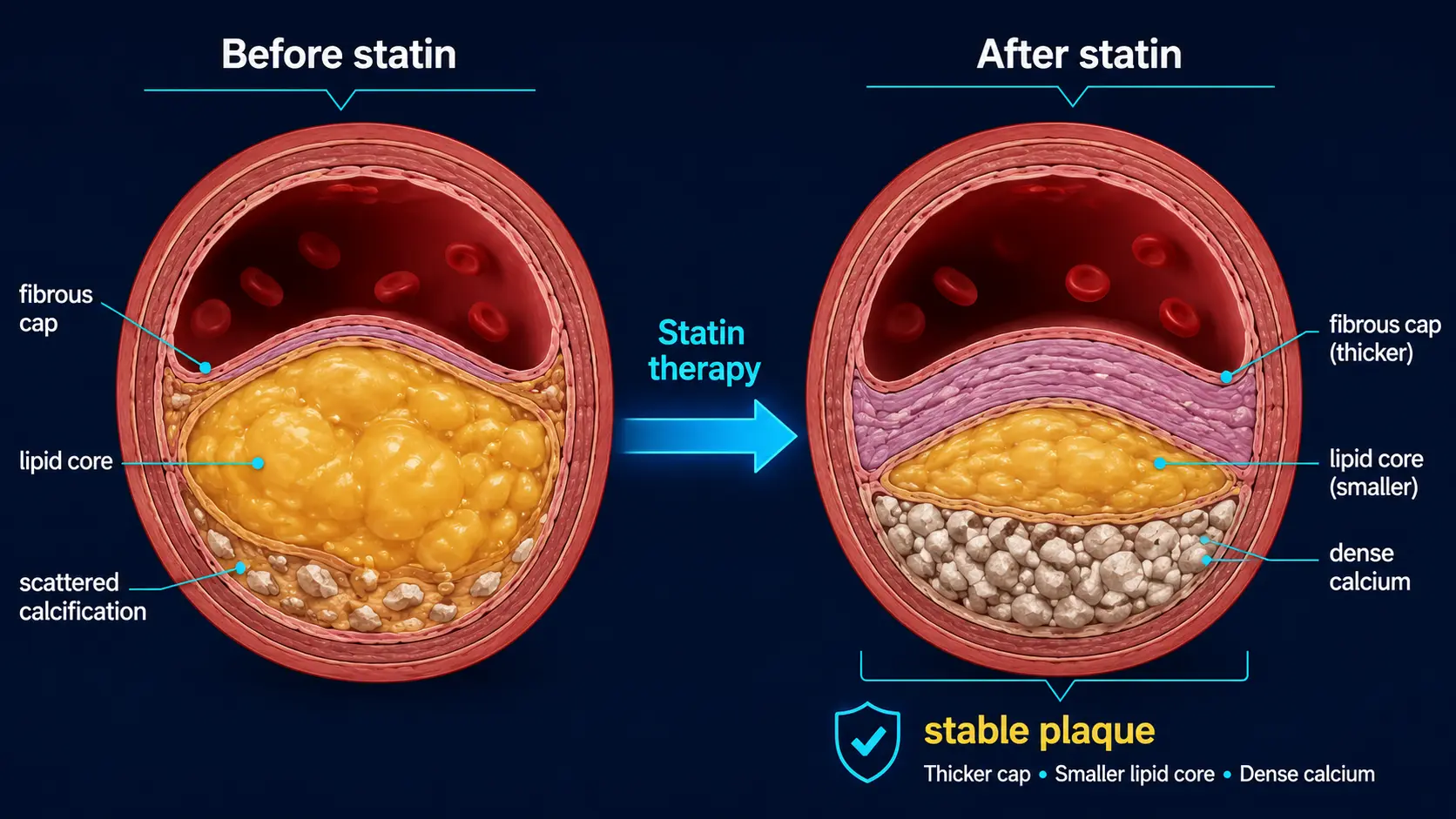
The Density Paradox
Here is the most counterintuitive finding in CAC research: statins make CAC scores go up.
Multiple randomized trials and registries have shown that patients on statins have higher calcium scores at follow-up than statin-naïve controls, despite having lower rates of cardiovascular events. The Agatston score rises (or progresses faster) on statin therapy by an average of 10–20% per year, more than the natural progression rate.
The mechanism is plaque stabilization:
- Statins reduce lipid accumulation in plaques and reduce inflammatory drive
- Stable plaques are more calcified than unstable plaques
- The body deposits calcium into existing lipid-rich plaque cores as part of the fibro-calcific stabilization process
- The Agatston score, which weights heavily toward dense calcium, captures this stabilization as an apparent "progression"
- Fewer plaque ruptures occur because the stabilized, denser plaque is less vulnerable
This is why a CAC score that has risen on statin therapy is not a signal that the medication is failing — it is, in many cases, a signal that the medication is working. Calcium volume scoring (rather than Agatston) tracks burden more directly and is sometimes preferred for follow-up. Either way, treatment decisions should be based on event risk and clinical context, not on a rising follow-up Agatston score in a statin-treated patient.
Progression on Statins
Practical interpretation of follow-up scans on statin therapy:
- Modest annual rise in Agatston score (10–20% per year) is expected; not a failure of therapy
- Stable or slowly-rising volume score is more reassuring than rising Agatston score because it isn't density-weighted
- Rapid increase (>30–40% per year) warrants reassessment of LDL/ApoB targets, medication adherence, lifestyle factors
- New high-risk vessel patterns (Left Main, proximal LAD) at follow-up may warrant additional imaging or stress testing
- Symptom development always overrides imaging trends — new chest pain, dyspnea, or exertional intolerance warrants prompt evaluation
The main reason to obtain a follow-up CAC on statin therapy is for patient motivation and adherence, not for treatment titration. A patient seeing their score rise from 200 to 300 over five years on a statin can be counter-intuitively reassured that this represents stabilization — if the message is delivered correctly. A patient who never gets a follow-up scan misses the opportunity for that conversation.
Beyond Statins
For patients with high CAC who tolerate or fail statin therapy:
- Ezetimibe — reduces intestinal cholesterol absorption; modest LDL reduction; good safety profile
- PCSK9 inhibitors (alirocumab, evolocumab) — potent LDL reduction (~50% on top of statin); injectable
- Bempedoic acid — pre-statin pathway inhibitor; useful in statin-intolerant patients
- Inclisiran — siRNA against PCSK9; twice-yearly injection
- Lp(a)-targeted therapies — in trials; pelacarsen and others may be available in coming years
- Aspirin 81 mg — consider if no bleeding contraindication, especially at very high CAC scores
- Lifestyle: see Reversal & Lifestyle
Research Papers and References
- ACC/AHA cholesterol guideline & CAC — PubMed search
- SCOT-HEART — PubMed search
- ROBINSCA — PubMed search
- Statin density paradox — PubMed search
- PCSK9 inhibitor outcomes — PubMed search
- Lp(a)-targeted therapy — PubMed search
Connections
- Coronary Calcium Score Deep-Dive Articles:
- CAC Overview
- Agatston Calculation
- MESA Calculator
- CAC = 0
- CAC vs Other Tests
- Soft Plaque Limits
- Reversal & Lifestyle
- ApoB
- Lipoprotein(a)
- Lipid Panel
- Cardiology
Featured Videos

Calcium Scores & Statins: What You Need to Know.

Coronary Calcium Score Test, Statins and the Risk of Heart Attack (When to use and How to interpret)
Do statins reduce heart scan scores?

Coronary Artery Calcium Score and Statins

EP 115 Coronary Calcium Score: A Prerequisite Before Statins? Insights with Dr. Paul Kolodzik

EP90: Can I Stop My Statins If I Have a Zero Calcium Score

Dr. Boz Reviews Guidelines on Cholesterol, Statins, & Risk for Coronary Artery Disease

Statins: Yes or No? Let this Test Decide

Statins, Calcium Score & CIMT vs Stress Test: Q&A with Dr Ford

EP90: Can I Stop My Statins If I Have A Zero Calcium Score?

What is a CAC Score? (Coronary Artery Calcium) Clogged Arteries? - 2026

5 Myths about the Coronary Calcium Score (CAC) | Tom Dayspring, MD

Coronary calcium score: what it means and how to interpret your results (AMA #5)

High Calcium Score: What Next?

Using the coronary calcium (CAC) score to predict cardiovascular disease risk | Allan Sniderman

What is a Coronary Calcium Score?